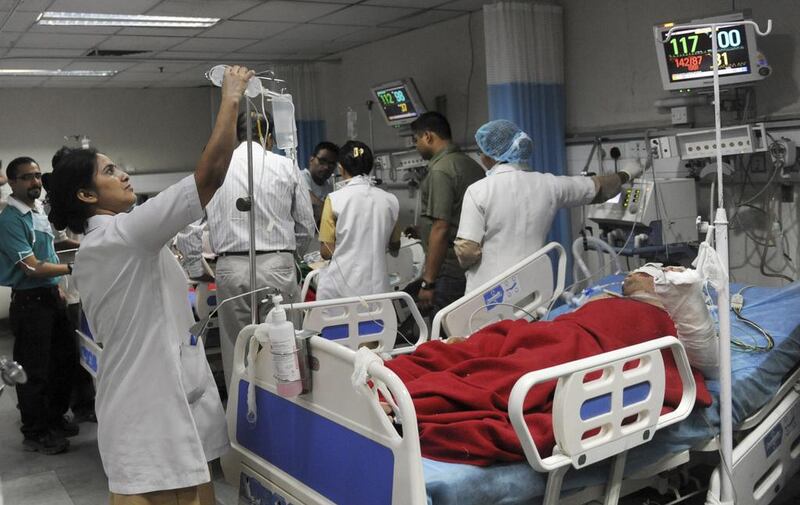
NEW DELHI // India’s creaking health infrastructure is facing one of its most dire challenges yet: a severe shortage of doctors and medical practitioners, which results in deficient care for hundreds of millions of people across the country.
According to the Organisation for Economic Cooperation and Development, India has 0.7 doctors per 1,000 people – lower than Pakistan’s 0.8, China’s 1.5, and the UAE’s 2.5.
The public health system, especially medical facilities in rural areas, bears the brunt of this deficit.
As of March 2015, 8 per cent of India’s 25,300 primary health centres had no doctor. More than 80 per cent of community health centres, where specialists practise, had no surgeons; 76 per cent had no obstetricians and gynaecologists, and 82 per cent had no paediatricians, according to a study by the Lancet – a UK medical journal.
The shortage comes despite India having more than 400 medical schools, which take in roughly 50,000 students annually. Even so, the country needs at least 750,000 more doctors, J P Nadda, India’s health minister, said in January 2015.
A large part of the shortage problem is that every year, thousands of doctors choose to leave India and study or practise overseas.
India-trained doctors account for nearly 5 per cent of American physicians and 11 per cent of British physicians, according to a 2005 study in the New England Journal of Medicine. According to OECD figures, nearly 86,000 doctors from India were working in the OECD’s 35 member countries. In second place were Chinese doctors, who numbered 26,000.
From April 2013 to March 2016, 4,701 graduates from Indian medical schools left to study or work abroad, according to the Medical Council of India, a government body that oversees medical education.
Of those who remain, most choose to work in cities, rather than move to rural areas, where the deficiencies of medical care are most glaringly felt. Private clinics and hospitals pay far more than government health centres, so newly minted doctors often follow the money.
Madhav G Deo, a Pune-based oncologist who has served on the Medical Council of India (MCI) – a government body overseeing medical education – said that the country’s foremost government hospital, the All India Institute of Medical Sciences in New Delhi, was always packed with patients.
“It’s like a crowded railway platform,” Dr Deo said. “Why are so many people standing around, having come from villages so far away? Doesn’t that indicate a failure of our system?”
In 2012, the Indian government decided that it should aim for a minimum doctor-citizen ratio of 1 to 1,000. At present, India has one doctor for every 1,681 people, according to MCI statistics.
But at that ratio, the pressure of work upon individual doctors can be intense.
Chandrakant Nair, who graduated from Pune’s Armed Forces Medical College in 2006, served a seven-year commission in the army as a medic before quitting both the military and medicine. He is now preparing for exams that will take him to business school.
“My parents are doctors also, and I’ve seen what their life can be like,” Dr Nair, who is based in the town of Nilambur, in Kerala, said. “I’ve seen how few family vacations we’ve been able to take, I’ve seen how they’re at the hospital virtually all the time.”
“I realised that, if you have to be a doctor in India, it means giving up any other interests you might have. And I didn’t want to do that.”
India needs to do a better job of training up its doctors, persuading them to serve in small towns and villages, and even convincing them to stay on in the profession, according to a 2013 report commissioned by Unicef India for the ministry of health and family welfare.
“Incentive packages ... must offer more than money to specialist doctors,” the report said.
“While housing allowances or housing quarters are provided for specialist doctors, the poor living conditions in rural areas are a major deterrent,” the report added. “[I]nvestments are needed to significantly improve infrastructure in areas of work and stay to significant[ly] incentivise specialist doctors to stay in rural areas.”
The report also recommended increasing the number of government medical colleges, and mandating rural postings or rotations for doctors.
India’s federal government considered making it compulsory for all doctors to serve for a year in rural India, but abandoned the plan last January, under pressure from medical bodies. Some states, such as Maharashtra and Odisha, do enforce stints of rural service upon doctors who have completed their undergraduate degrees.
Dr Deo thinks it is a good idea to work a mandatory rural posting into a doctor’s training programme, but he holds different views about the deficit of personnel itself.
“I don’t agree with this 1:1,000 ratio,” he said. “You know how they came up with that? By defining a doctor as someone who administers measles vaccines or delivers a baby. You don’t need a doctor to do that. A paramedic or a nurse or a midwife can do those things.”
The government’s primary health centres in rural India do need more paramedics and nurses, Dr Deo said. But India’s villagers now increasingly need more specialists rather than general physicians, he added.
“Diabetes and heart disease and cancer are on the rise, and you need doctors to tackle those diseases, not ailments like diarrhoea or fever, which can be treated even by a well-trained nurse,” Dr Deo said.
Instead of opening hundreds of medical colleges, India would be better served training more supplementary medical staff and opening large hospitals in smaller towns, which are accessible by nearby villages, he said.
“There’s a lot of interest in opening more colleges, because of the money that can be made off them,” Dr Deo said. “But that’s not what’s needed. What’s needed is a rethinking of how medical education works, and to review the structure of health care altogether.”
ssubramanian@thenational.ae