The way Munira Abdulla defied expectations and began communicating with family more than a quarter of a century after she suffered devastating brain damage has made headlines worldwide.
As reported in The National this week, Ms Abdulla ended up in a minimally conscious state (MCS) after a collision between the car in which she was travelling and a school bus. She was aged 32 at the time.
For 27 years she was unable to speak to her children until last year when, after intensive treatment in Germany funded by the Crown Prince Court, she showed a dramatic improvement. While still severely disabled, she can now answer questions and recite verses from the Quran.
Although Ms Abdulla’s case offers hope, emergence from MCS remains “very uncertain”, according to Professor David Wilkinson, a professor of psychology at the University of Kent in the United Kingdom who researches therapies for brain-injured patients.
Typically, the longer someone is in a MCS, the less likely it is that they are “going to make a full recovery or a recovery that offers a real richness of life” said Prof Wilkinson. “But you do get exceptional cases.”
Dr Mary Braine, a senior lecturer at the School of Health and Society at the University of Salford in Manchester, has “nursed many” patients with brain injuries during her career.
A key challenge, she said, was achieving an accurate diagnosis, and some cases around the world that have hit the headlines may have involved misdiagnosed patients.
A person in a coma shows “no signs of being awake or being aware”, according to the UK’s National Health Service.
A coma typically lasts just a few weeks, after which time the person may move into being in a vegetative state or a minimally conscious state.
Someone in a vegetative state is awake “but showing no signs of awareness”, although reflexes may work, with the patient removing their hand if it is squeezed hard. After a few weeks the vegetative state is described as persistent or continuing and, after a number of months, permanent.
Minimally conscious patients are slightly more responsive, showing “clear but minimal inconsistent awareness”. Some will, at times, respond to commands, perhaps by moving a finger, or they may even be able to communicate.
A separate condition is locked-in syndrome, often caused by a stroke. Consciousness is not impaired, but the person is paralysed and only eye movement might remain.
“With full locked-in syndrome, potentially there’s an element of the person being seen as being in a minimally conscious state or low-awareness state when they’re not,” said Dr Braine, who described the syndrome as a “terrible, awful” condition because the person remained fully aware.
Assessments of people with brain injuries typically rely on looking at their outward behaviour, but research has indicated there may be “some degree of awareness and internal activity that we simply don’t know about”, said Prof Wilkinson.
“When you put some of these individuals in a brain scanner and ask them questions, you’ve got patterns of brain activities similar to those who aren’t in MCS,” he said.
“Some of these individuals are experiencing life and their surroundings in a far richer way than we anticipate.”
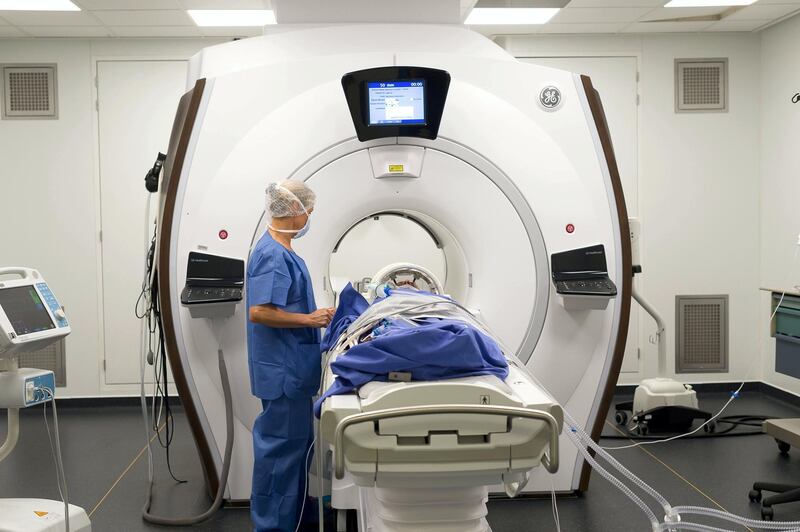
In one case, researchers used functional magnetic resonance imaging (fMRI) - which measures the brain’s electrical activity - to assess a man diagnosed as being in a permanent vegetative state after a car crash in 2003.

The results indicated that the man could understand, and answer correctly, questions about his family.
Campaign groups, such as the organisation Care Not Killing, have said such findings, and instances where dramatic improvements in consciousness are seen, show that food and water should not be withdrawn from patients in a permanent vegetative state or a minimally conscious state. The issue of withdrawing care has sparked controversy and resulted in court cases in a number of countries.
“It feels like an area of medicine where our understanding is improving,” said Dr Gordon Macdonald, Care Not Killing’s CEO.
“It seems premature to make decisions to withdraw food and fluid for people when there’s a possibility they might recover or improve.”
While the prognosis for brain-injured patients often remains uncertain, and with drug therapies having “chequered efficacy”, researchers such as Prof Wilkinson are trying new approaches.
His work has involved stimulating the patient’s balance system by applying a modest electric current behind the ears or gentle heating inside the ear canal. The balance system may be key because “its tendrils run far and wide”.
“In the case of MCS, quite often the injury is quite diffuse and runs far and wide [too],” he said, adding that with two individuals, “dramatic improvements” have been seen with the technique. However, a lack of funding has limited the number of people the technique has been tried with.
Prof Wilkinson said efforts to bring people with debilitating injuries to an increased state of awareness raised ethical questions, since this gives them “awareness that they cannot do what they want to do”.
“Is it better to come out of MCS and be functionally disabled and have some quality of life, but potentially be depressed?” he said.