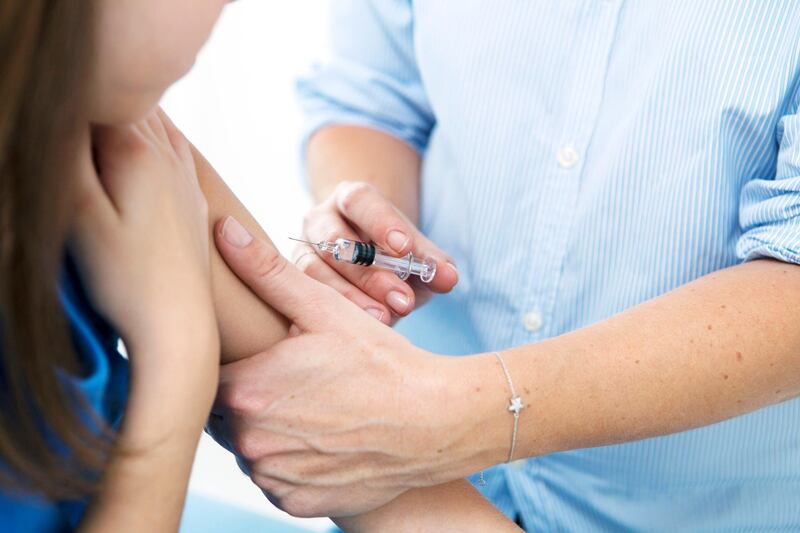
Deaths from cervical cancer are set to almost double in the next 15 years, according to a new report that demonstrates the urgent need for women to get tested.
The Journal of Infectious Diseases said 9,930 people died from 19,500 cases in in 2015 in the Middle East and North Africa.
This is estimated to rise to 18,850 deaths from 33,700 cases in 2035.
In some countries including Morocco and Saudi Arabia, about one in four have human papillomavirus (HPV) owing to low societal awareness and low screening rates.
“It’s important that wherever there’s progress in tackling NCDs, we learn from it and scale it up across the world," said Dr Sania Nishtar, co-chair of the WHO’s Independent High-Level Commission on Non-communicable Diseases.
“For too many women, life is being cut short by cervical cancer."
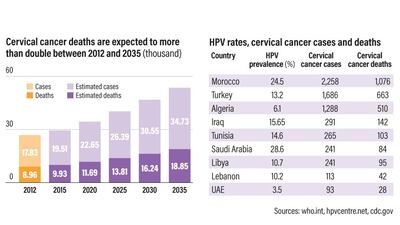
Introducing a vaccine against HPV in childhood immunisation programmes in the UAE has helped drastically reduce the number of women with cervical cancer.
The free vaccine was first offered to girls in school settings a decade ago in Abu Dhabi, reducing the number of women with the cancer.
Abu Dhabi is leading the fight against cervical cancer and provides a roadmap for others to follow, campaigners said.
The Journal of Infectious Diseases has said the HPV rate in women aged 18 to 24 dropped from more than one in five women to approximately just one per cent.
“By investing in women’s health, especially in preventative care, nations are investing in their future prosperity,” said Mychelle Farmer, Chair of the campaign group NCD Child.
“If women have access to good quality health services, then they and their children are much more likely to stay healthy and contribute positively to their nation."
Cervical cancer kills more than 250,000 women worldwide every year and there are at least half a million new cases reported globally.
The virus causes virtually all cases of cervical cancer, approximately 70-75 per cent of vaginal cancer cases and about 30 per cent of vulvar cancer cases in females.
It is estimated approximately 530,000 women develop cervical cancer annually around the world, with about 85 per cent of cases occurring in developing countries.
Cervical cancer affects women in all countries, yet this preventable disease is the second largest cancer killer of women in the Middle East and North Africa region.
__________________
Read more:
Emirati boy among first in region saved by non-surgical heart procedure
Nine out of ten cancer cases 'could be prevented with smear test'
___________________
Libya also introduced the HPV vaccine in 2013 as part of its National Immunisation Program and is currently considering offering it to boys and girls, whilst Australia is a model of how to effectively roll-out a comprehensive package of HPV vaccines, screening and treatment.
The MENA Cervical Cancer Crisis Card campaign has been launched in the region, to encourage other countries to improve their own screening protocols.
The campaign is encouraging a rollout of a comprehensive approach to cervical cancer that includes HPV vaccines to prevent the disease, and more regular screenings to detect HPV and cervical cancer.
Increasing early screenings using methods such as pap smears, colposcopies or visual inspection with acetic acid (VIA) to help diagnose precancerous cells.
Early detection can encourage quality treatment to prevent precancerous cells from growing, offering hope to the hundreds of thousands of women who missed out on the vaccine.
It is also calling for health systems to be strengthened so that all women can access affordable treatment and quality care.
“The MENA Cervical Cancer Crisis Card highlights that urgent action is needed to prevent HPV infections and death,” said Batool Alwahdani, vice president of external affairs, of the International Federation of Medical Students Association.
“By scaling up a comprehensive approach to vaccination, screening and treatment, we can rewrite history and move towards the global goal of eliminating HPV.”