Despite all its record-breaking triumphs and towering achievements, the UAE still has many formidable challenges to overcome.
One of these is reducing the worrying number of people who are diagnosed with type-2 diabetes, the lifestyle disease caused by excess body weight and lack of physical exercise.
In fact, the UAE regularly finds itself among the countries with the highest percentage of the population with this condition.
However, advances are being made, with the government ploughing resources into treatment and awareness programmes. While four years ago, according to the World Health Organisation (WHO), the Emirates had the second-highest rate of diabetes in the world, recent statistics reveal that it has now fallen to a less unsettling 10th.
Despite this improvement, between 20 and 25 per cent of adults in this country still suffer from type-2 diabetes.
This effectively means a sizeable chunk of the population face life-threatening conditions, such as cardiovascular disease, limb loss and kidney failure.
Diabetes is also the world’s leading cause of blindness for people of working age, with the WHO estimating that after 15 years, approximately two per cent of sufferers become blind and about 10 per cent develop severe visual impairment.
This condition has been one of the government’s most pressing concerns, with the Ministry of Health investing heavily in state-of-the-art eye-care facilities to such a degree that cases of severe diabetic retinopathy have almost halved in the past two years.
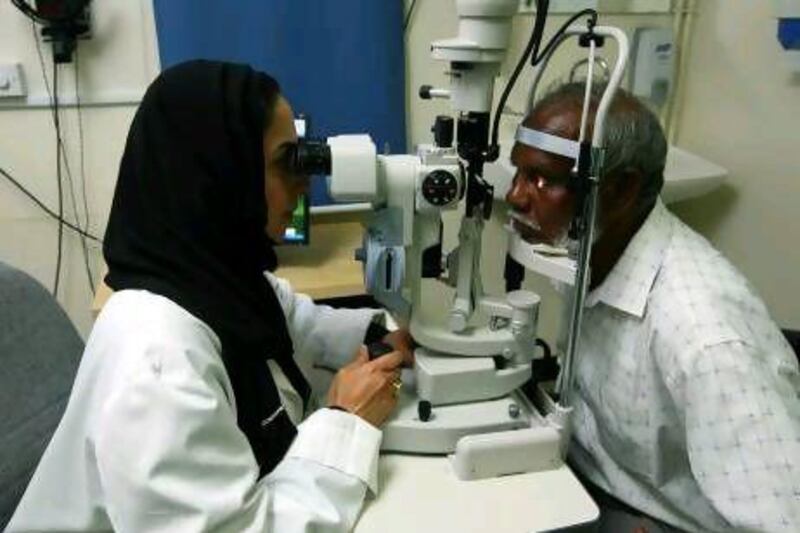
Dr Manal Taryam, an Emirati ophthalmology consultant with Dubai Health Authority, who also served as vice president at last month’s World Ophthalmology Congress in Abu Dhabi, is at the forefront of this campaign.
Speaking to her after the congress, she talks passionately about the medical advances that have put the UAE at the cutting edge in detecting and regulating the ailment.
“These days, diabetes is not a disease that should lead to disability. It can, and it does, [but only] if people allow it to,” she explains.
“Up until a few years ago, we were continually dealing with patients who were [rendered] totally blind by diabetes. Thankfully, this is a very rare thing today.”
Despite this, a significant number still showed diabetic tendencies: “We are still getting patients who are coming to us with visual impairment and then when we look into their eyes we see signs of diabetes retinopathy.
“And when we ask them if they had diabetes, they say ‘no’. So they were never diagnosed. They’re not aware that they have the disease. These are the lucky ones who we actually get to in good time, but it shows we have more work to do.”
These causes are simple enough. Type-2 diabetes is a slow, insidious disease that creeps up on overweight or unhealthy adults, as their poor health affects their ability to regulate the insulin in their body.
Thus, their blood is packed with excess blood sugars, which slowly erode the walls of the blood capillaries in the back of the eye. This continuous damage means the tiny vessels begin to haemorrhage plasma and proteins and lipids into the eyeball, resulting in blurred vision.
The body responds by forming blood clots, scars and new blood vessels, which manifest themselves as blotches in the line of vision. In the most serious cases, the clotting will eventually cause the retina to detach, resulting in permanent blindness. The speed and nature of how the disease spreads depends on where it forms in the eye.
Dr Taryam says: “How quickly [the visual impairment] develops depends on where it starts. If it’s in a central part of the vision, where it is more noticeable, when you are reading, you see the lines moving up and down and they’re kind of zigzagged. Or if you look at a door, it’s not straight.
"If it affects the periphery vision, it can creep in from the sides, which is more dangerous as this can happen slowly over the years. When this happens, when they finally come to us, sometimes it's too late and their vision cannot be saved."
To prevent this happening, Dubai Health Authority and its counterparts in other emirates have enacted a number of far-reaching schemes. One of these is telemedicine, where patients have their eyes and blood sugar levels examined at their GP surgeries, then the results are transmitted to their ophthalmologists and endocrinologists. If the level of blood vessel damage is reaching dangerous levels, the patient is called in for treatment and advice.
Dr Taryam explains: “In this way, we are detecting the early cases, meaning that the number of cases of diabetes-related retinopathy has at least halved in the last two years. Because of this, the state of their eyes can be acted upon immediately. Plus we get information about how they’re controlling their blood sugar levels.”
Dr Taryam believes the UAE’s treatment of the disease is equal to, if not better, than anywhere in the world.
She claims: “I’ve worked in Germany and the medicinal care we have here is just as good. Because the country is small and is connected by the Ministry of Health, we can make sure that people are immediately referred. So we all know each other in our profession and we’re all working together for a common goal.”
Medical progress is also being made in surgical techniques, such as laser treatment to cauterise the damaged vessels in the eyes and prevent further bleeding. But Dr Taryam insists these are just a last resort, and often do nothing more than slow down the proliferation of the disease. So, the strict regulation of blood sugar levels is still the most effective cure.
“I tell my patients ‘your eyes are the victims of diabetes, not the cause of the disease. So you have to help me treat you. If you don’t control your blood sugar, we start from square one again’,” she explains.
“There is a limit to how much [retinal damage] an eye can take. We can treat, but then we are losing cells every time you get a haemorrhage or a retinal detachment. We have to reiterate to the patient that they must cooperate by controlling their blood sugars as well.”
The fear of losing one’s sight is usually enough to affect change in their living: “You know, it is terrifying for people to think they might lose the gift of vision, so once we’ve spelt out the dangers, the patient generally starts to make these changes.”